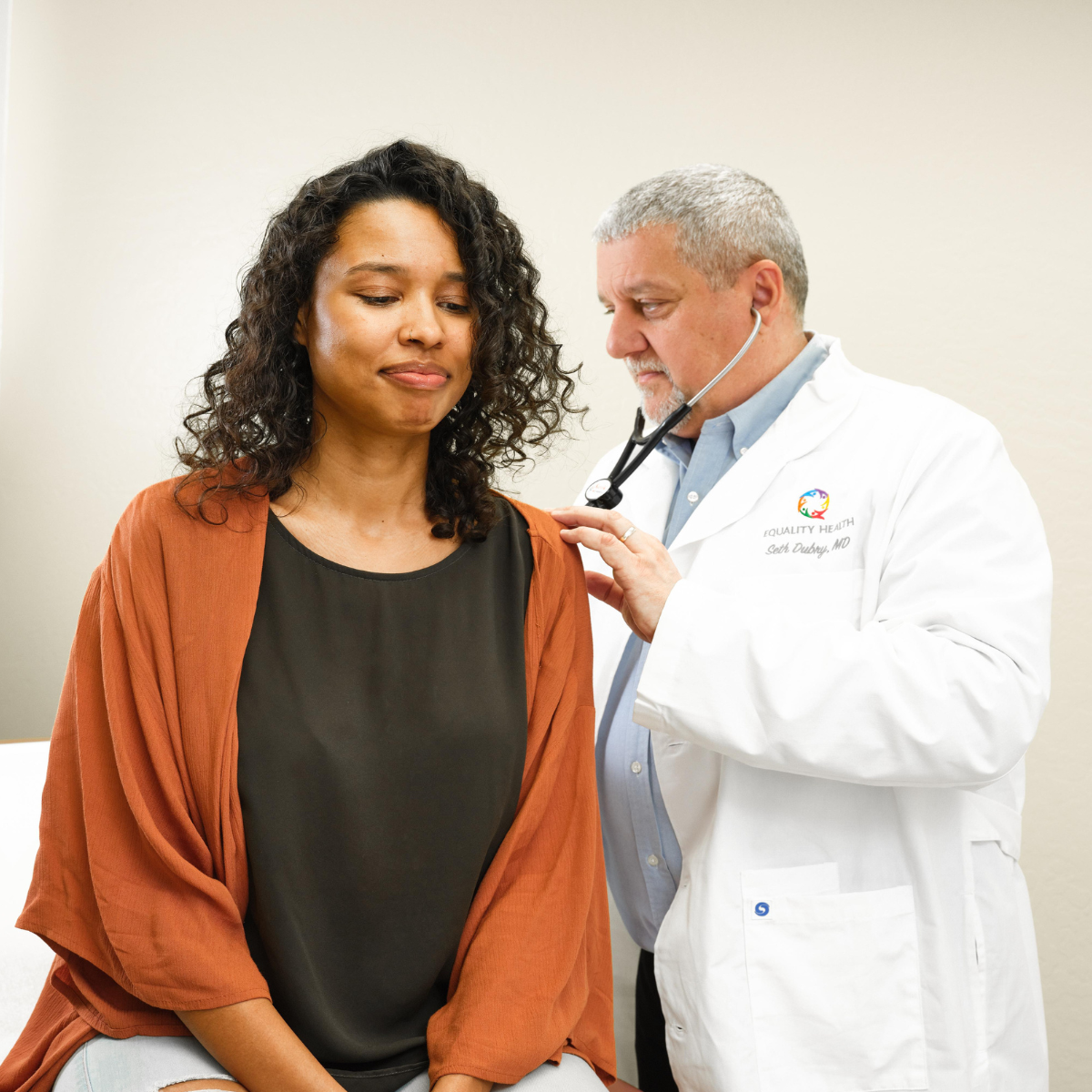
Did You Know That Social Risk Factors Have More Than Twice The Impact On Outcomes Compared To Clinical Care?
Our healthcare system as it functions now is not equipped to address SDOH, and with heavy administrative burdens, doctors and nurses are often left with too little time with patients to recognize social risk factors and often lack the resources, knowledge and comfort level needed to screen and connect patients with necessary supports.
Social risk – language barriers, air quality at home, transportation limitations – have a 50% impact on health outcomes, compared to just 20% for clinical care. So why is it that 4 out of 10 patients in higher risk communities are still rushed out of doctor’s offices, much less screened for social risk?
The answer probably is due to a lack of education and support for the frontline health workers, physicians and nurses, and a broader challenge of establishing a true medical home for the Medicaid population. Consider, for starters, that life expectancy gaps in neighborhoods within the same city can be as drastic as 30 years as a result of socioeconomic conditions negatively impacting health outcomes – things like poverty, low literacy, and highways separating housing and access to a grocery store. These conditions are now labeled as social determinants of health (SDOH) and while the label may be relatively new, the conditions are not:
- Individuals living in poverty have higher death rates for the 14 leading causes of death
- Over 34m people in the US experience food insecurity, which has been associated with increased risk of diabetes, heart disease, obesity and other chronic conditions
- ~1/3 of homeless individuals have a serious mental illness and homelessness is on the rise, having increased +6% between 2017-2022
Forty percent of consumers surveyed by BRG indicate having felt rushed out of a doctor’s office in the past
One Medicaid patient – Saul, a 55 y/o male – gets blood work done that indicates high cholesterol. At Saul’s follow up appointment his numbers are still elevated, so the doctor, assuming that the drug isn’t working, switches him to a different statin. What the doctor did not know – nor ask because he had to run to his 10th 15-minute appointment of the day – was that Saul had skipped doses because he couldn’t afford the medication and Saul never adjusted his diet as recommended. Saul will more than likely continue to return to follow-ups with elevated numbers. Eventually, he may come across a doctor who has the time and resources to set him up with necessary supports to change behavior and lower those levels, or maybe he will spiral in and out of the hospital.

Through Medicaid demonstration waivers, states can permit Medicaid MCOs to offer social supports, but this isn’t a fix on its own. It’s a step in the right direction that an MCO may pay for mold removal or ventilation improvements in the home of an asthmatic child to prevent a future emergency room visit, but a PCP may not recognize that this is allowed or even needed over something more clinical like a nebulizer to alleviate asthma symptoms. Efforts to educate PCPs on how to identify social risk factors and incent them to do it consistently are necessary steps.
“A relationship with a primary care provider is implied at best, and there’s a portion of the Medicaid population not even engaged with a care provider.”– Family Medicine Doctor
Screening for SDOH is a key first step in addressing inequities. Performing screenings in the home is ideal, as some nonprofits do. Doing them in the PCP office is now thought to be important to help physicians tie social risk to health risk, but there are gaps. A portion of the Medicaid population are not even engaged with a PCP, and even when they see patients, practices report a lack of training to do the screening and resources to act on situations when the patient has risk. “It’s not as simple as a PHQ9 – there’s a cultural sensitivity and often a barrier – we have tried to bring in interpreters but don’t get the reimbursement for it,” Anita Florez, APRN, said.

SDOH screening systems are used primarily at this stage to collect data rather than connect patients with support services. Medicaid MCO Priority Health has leveraged Z-codes to determine how many of their members have social risk. This is a start, but there is some debate about which codes to use (e.g. Z codes or LOINC codes) and how to use the data. For PCP groups, it will be important for payers and their partners to develop a uniform system for screening and reporting. “It would be nice,” Florez said, “if we could have one screen and if we could get help staffing this function – someone to work with nurses and follow up with patients – in the form of a social worker embedded in the practice.”
Stakeholders will need to work together to make a lasting impact. In Dallas, a collaborative effort brought housing, community gardens, a healthy market, medical and social support, and remote monitoring to a historically Black neighborhood just south of the Trinity River in east Oak Cliff. Pastor Vincent Parker spearheaded the effort with funding for housing from the Golden SEEDS Foundation, the community development arm of the Golden Gate Missionary Baptist Church. More of these local investments in social and health infrastructure are emerging, but to make them stick there will need to be measurement-based care that includes SDOH screening coupled with medical monitoring.